By Hannah Shub, Jordon Pfeiffer, Leon Tomlinson, Maria Jose Solis Prado and Olivia Gil

During a 12-step meeting in Pinellas Park, Florida, an attendee began to slow down. His breathing became shallow, his pulse faint, his words slurred.
Ryan Conz, a former nurse technician with more than a decade of experience, didn’t hesitate.
“I went into nursing mode,” Conz said. “I treated him as a patient. I kept calm. I already knew what to do.”
While Conz didn’t administer it himself, he directed the process, telling the one administering that the patient needed one hit of naloxone, then two more hits.
“He’s still alive,” Conz said.
That moment, a life interrupted but not ended, is what overdose prevention workers across Pinellas County say is now at risk.
As of late 2024, the Statewide Council on Opioid Abatement Annual Report document outlined Florida’s newfound funding priorities. According to the report, the $250,000 that the state provided annually to independent outreach efforts, overdose prevention and naloxone distribution would no longer be provided.
The long-term impact of the funding decision remains unclear. Despite the decrease in fatal overdoses attributed to accessible naloxone, an effective opioid reversal drug, local independent harm reduction collectives still face setbacks from funding cuts.
“You might think we’re saving a few bucks,” Becca Smith, the program and outreach specialist at the Florida Harm Reduction Collective, said. “But in reality, you’re really not saving money. You’re playing with people’s lives.”
The Florida Harm Reduction Collective (FLHRC) is an independent, non-profit program that specializes in public health safety and harm mitigation. From naloxone distribution, clean syringe services and fentanyl test strips, the FLHRC is just one of many overdose prevention organizations that suffered from the state budget cuts of 2024.
“Our salaries were funded, but our supplies this year were not,” Emily Fuchs, the program manager at the FLHRC, said. “And we’re expected to go out there with no supplies and no incentives and no money for transportation. So, we’ve had to continue to seek funding in other places or pull funding from other sources.”
For both Fuchs and Smith, the shift in funding is not theoretical, noting the impacts they have seen happening among the community.
“People are already dying now,” Fuchs said. “People certainly will die if they continue these cuts. These are compounded issues. These are systematic issues. Someone’s homeless, they’re at higher risk. Someone uses drugs, higher risk. They have an infection, now their risk is even higher, and it keeps going and going.”
To understand what happens when prevention infrastructure shrinks, Dr. Khary Rigg, a professor in the Department of Behavioral Health Science and Practice at the University of South Florida, points to how funding decisions shift the burden.
“These dollars determine whether jurisdictions can be proactive or whether they’re constantly in crisis response mode,” he said.
When prevention programs are reduced, first responders and emergency rooms absorb the pressure, he explained.
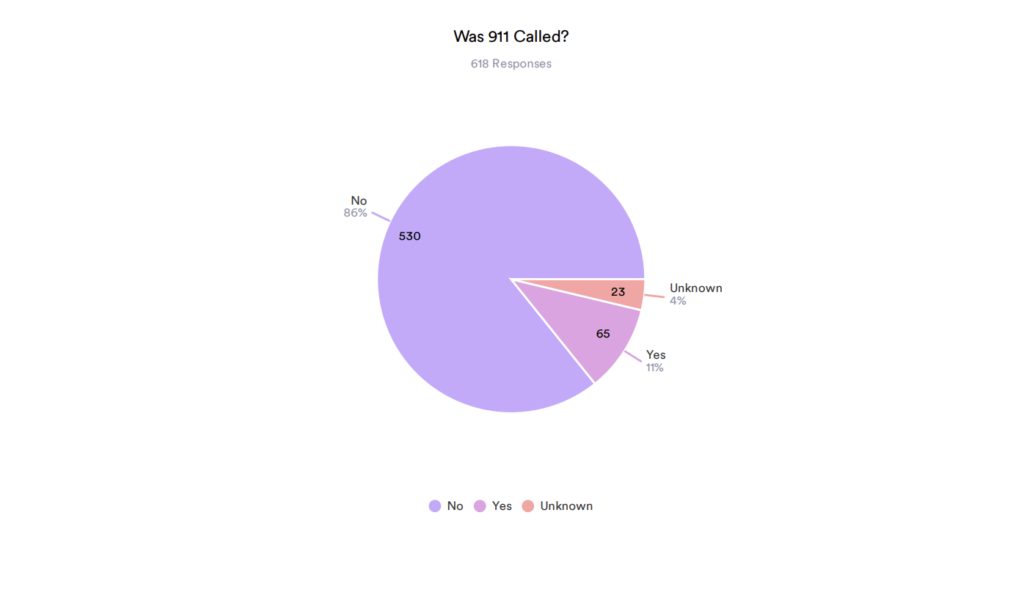
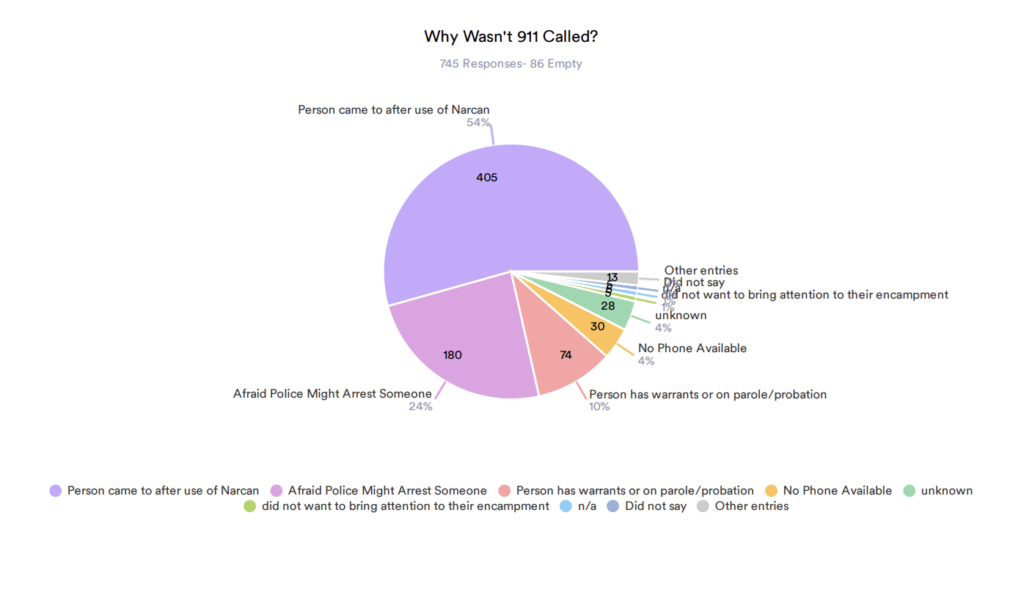
“First responders, EMS teams, emergency rooms and law enforcement are the ones who experience the higher burden when prevention programs get cut,” he said. “They [policymakers] see it as a quick fix, but in reality, it ends up being more expensive.”
While some data advocates that overdose fatalities are on the decline, both FLHRC workers and Rigg advise against believing all the numbers. Smith explained that many of the fatalities remain unreported, specifically, deaths occurring in unhoused populations.
“If you overdose in the fancy neighborhoods in South Tampa,” Fuchs added. “It’s going to get counted, but not our folks under the bridges and in the encampments. Overdoses are down, that’s true. But our people aren’t counted.”
Rigg furthered Fuchs and Smith’s sentiments, noting the lag in official overdose data.
“By the time it becomes publicly available,” he said. “It’s six months, a year or a year and a half out.”

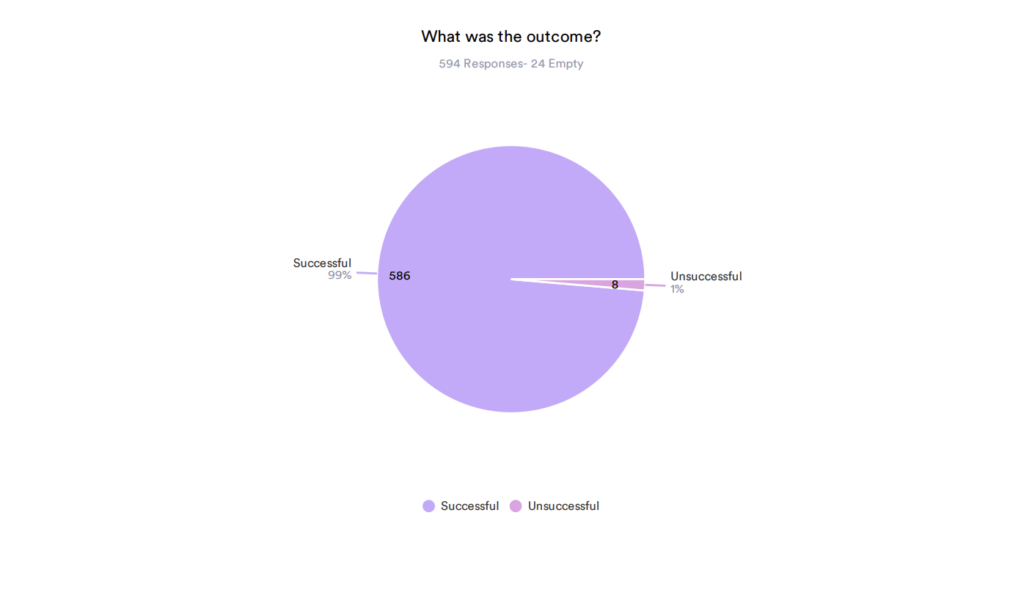
Conz witnessed that unreported data in real life.
“I know a lot of people that are still alive because of Narcan,” Conz said.
He estimates the medication can begin working within four to five minutes, sometimes faster depending on the substance involved.
“If they shut this off,” Conz said, referring to distribution cuts, “a lot more people are going to be dying.”
Furthermore, Rigg hopes for naloxone to maintain a steady, high supply within its distribution. He describes naloxone’s place in urban, rural or suburban communities as “non-negotiable.”
“Narcan saves lives. Period,” Rigg said. “It is one of the most rigorously studied and consistently effective public health tools that we have to lower overdose risk. Narcan democratizes life-saving intervention.”
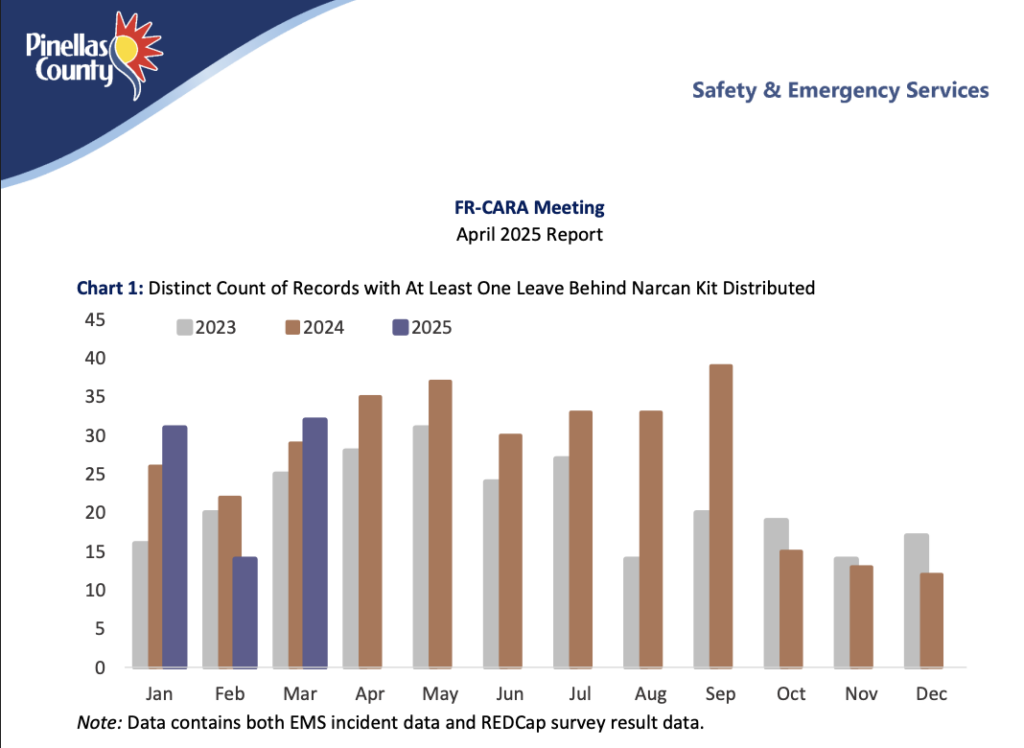
Between Conz’s real-life account, Rigg’s thorough research and the FLHRC’s hands-on endeavors, the annual funding loss effects on overdose prevention efforts become more and more clear. While the long-term impact is still forthcoming, the short-term influence is evident.
“It can happen anytime, anywhere, to anyone,” Fuchs said. “These are living, breathing, feeling, loving people. They’re someone’s mom, dad, brother, sister.”
For the FLHRC, overdose does not discriminate by income, profession, or neighborhood. It does not announce itself ahead of time.
“We don’t need to be funding what makes us comfortable,” Rigg said. “We need to be funding what works.”



